DVT
A recent systematic review showed that emergency physicians are just as accurate as radiologist for finding DVT (1).
For point of care, the main concern is whether there is a thrombus in the proximal deep veins: Common Femoral (CFV), Femoral (FV) and Popliteal veins. If I see a very proximal clot eg CFV, I also look at the iliacs, IVC and right heart to complete the picture.
The aim of the DVT US:
1. Image the deep veins in trans
2. Assess the echogenicity of the lumen
3. Assess compressibility
Acute thrombus in the lumen leads to inflammation and can cause the fat surrounding the vein to appear hyperechoic. This can be your first clue that something bad is going on.
I use the abdominal probe for most DVT scans because it has a wider field of view and has great superficial resolution. With the linear probe, it's easy to lose the vein as it travels deeper in the thigh.
Anechoic lumen + Compressible = No DVT
POSITIONING THE PATIENT
If you have time, put the bed 30 deg in reverse trendeleberg to cause some degree of LL venous engorgement.
Have the leg abducted and slightly flexed at the hip and knee.

Leg position: R leg for CFV and FV; L leg for pop v
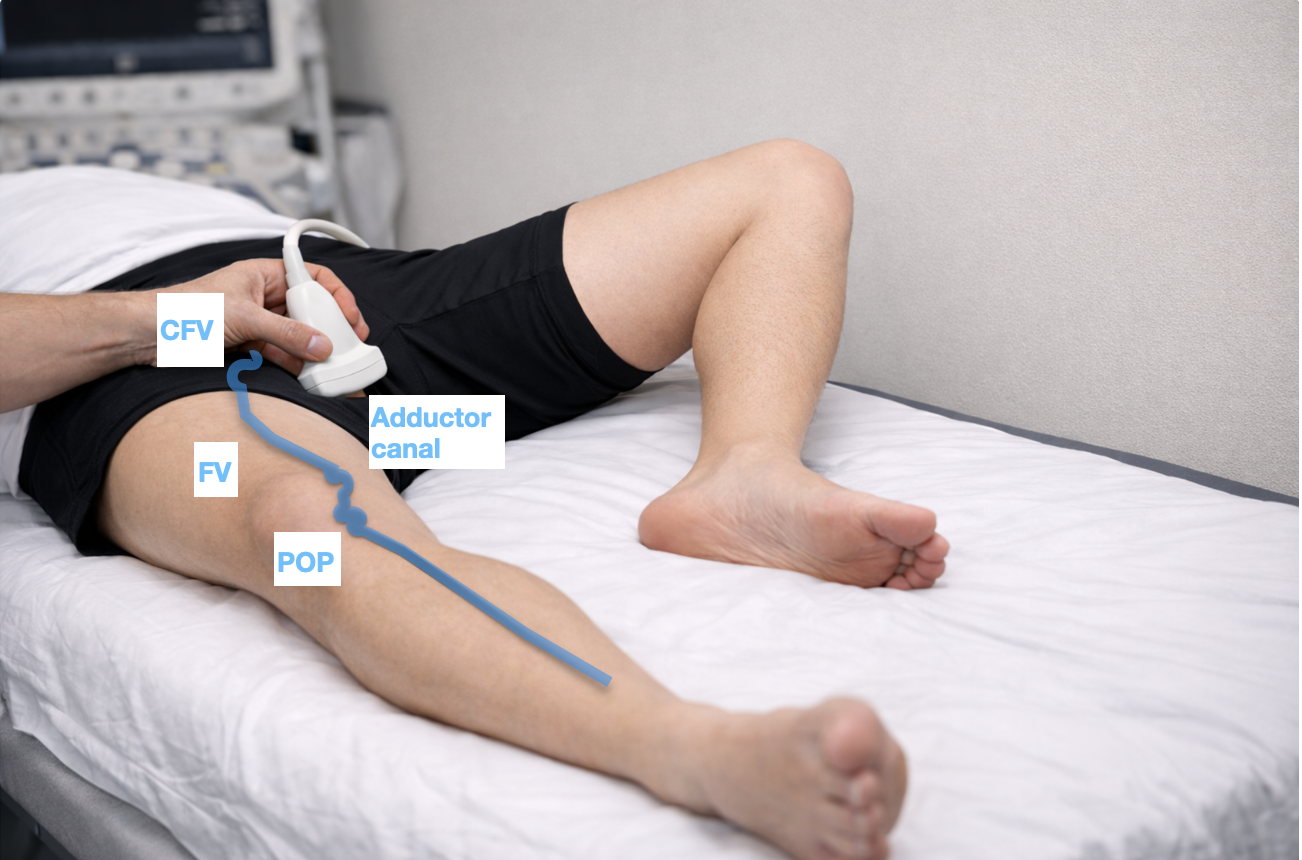
Position of veins on the leg. At the adductor canal, the FV passes under the sartorius muscle
TECHNIQUE
There are POCUS articles out there advocating 3 point and 2 point compression for DVT POCUS. 3 point compression is compressing the vein at CFV (inguinal triangle), FV (mid thigh) and popliteal (behind the knee). Two point is where you skip the FV compression. The traditional teaching is that two point compression can miss the 5% of DVTs isolated to the FV (2). But a recent meta-analysis has debunked this (3)
In radiology, the entire vein is visualised from the CFV to the popliteal and compressed at 1-2 cm intervals. This is what I do and it doesn't take more time. With the 3 or 2 point compression, you can spend time trying to find the vein again.
To assess the vein: apply a strip of gel on the medial thigh from the inguinal canal to the knee. Hold your probe in transverse with the probe marker to the patient's right. Hold the probe as close to the face of the probe as possible and stabilise your palm on the patient's leg.
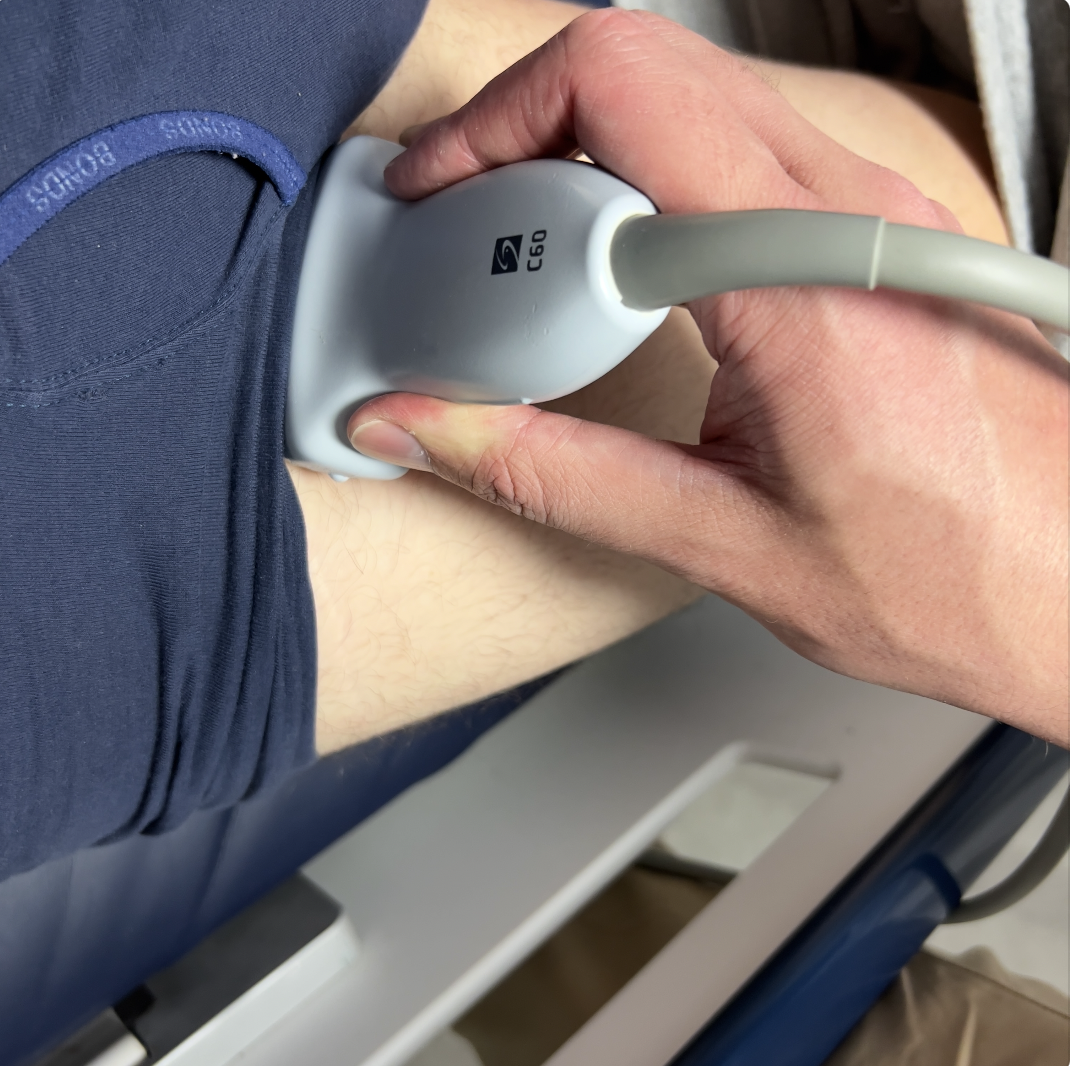
Once you find the vein change the screen to "dual screen" to make it easier to save the normal and compressed images side by side. To save a dual image: image the vein, freeze, tap on the split screen on the right, compress the vein, freeze and then take a still of the dual images. Label these as comp/non comp depending on the pathology that you find.
COMMON FEMORAL VEIN
Find the CFV in the inguinal region and image it at its origin. This is where the long saphenous vein joins it medially.
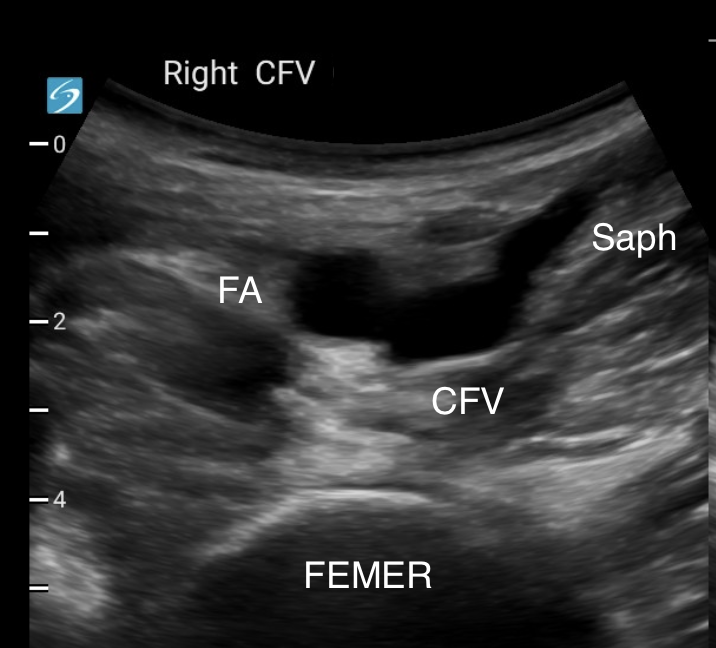
Compress the vein against the femur by putting downward pressure on the probe while keeping the vein in view. It's easy to lose sight of the vein by accidentally fanning cranially or caudally when you do this. That's why it's important to stabilise your palm/wrist on the patient's leg.
A normal vein will compress so that the lumen completely disappears.
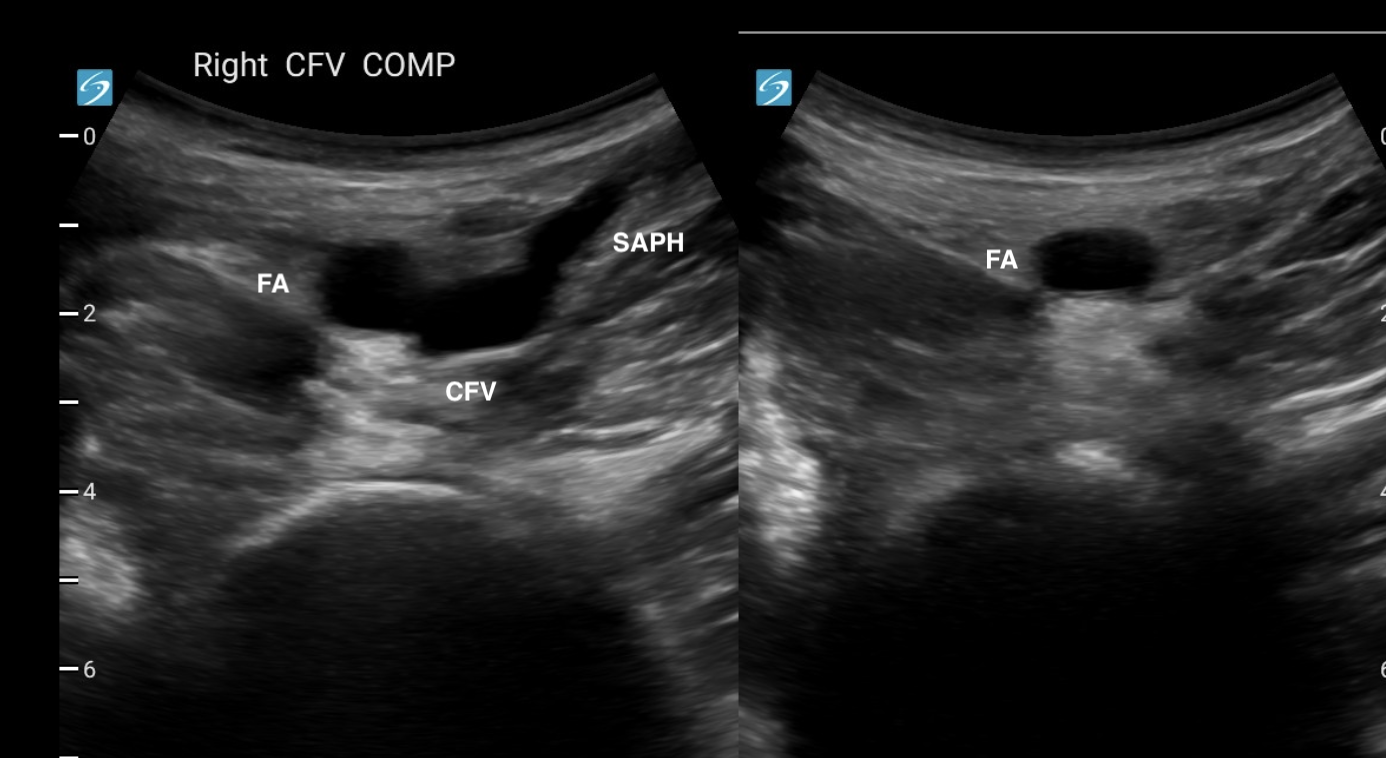
The image on the right only shows the FA, because the CFV and saphenous vein have been compressed.
FEMORAL VEIN
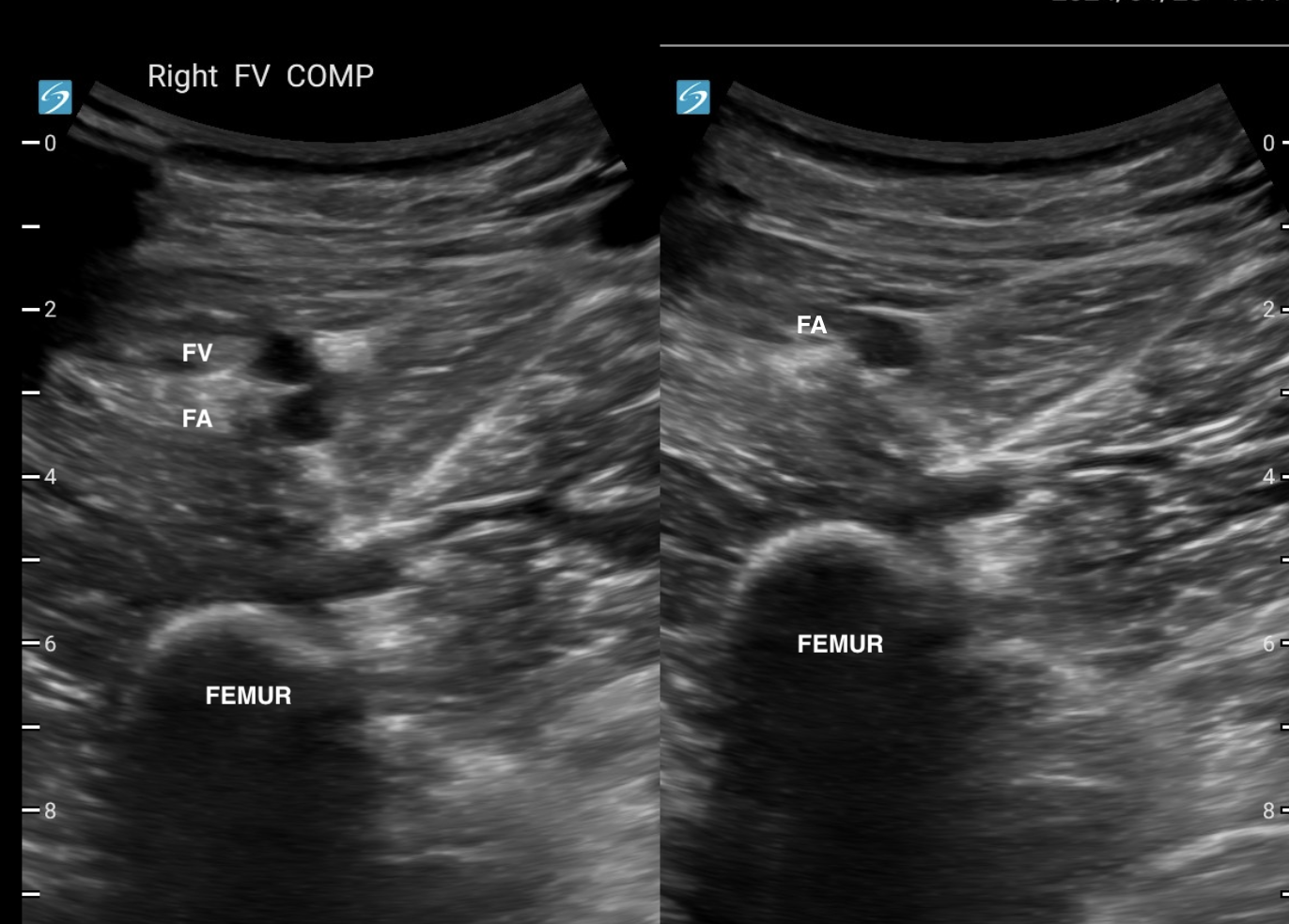
The femoral vein travels medially down the leg and passes under the sartorius muscle at the adductor canal. Mostly it can be compressed with downward pressure. At the adductor canal, have the probe facing the medial femur and compress the vein against the femer by putting lateral pressure. At this point, you may need to help with medial pressure from your hand against the patient's lateral leg.
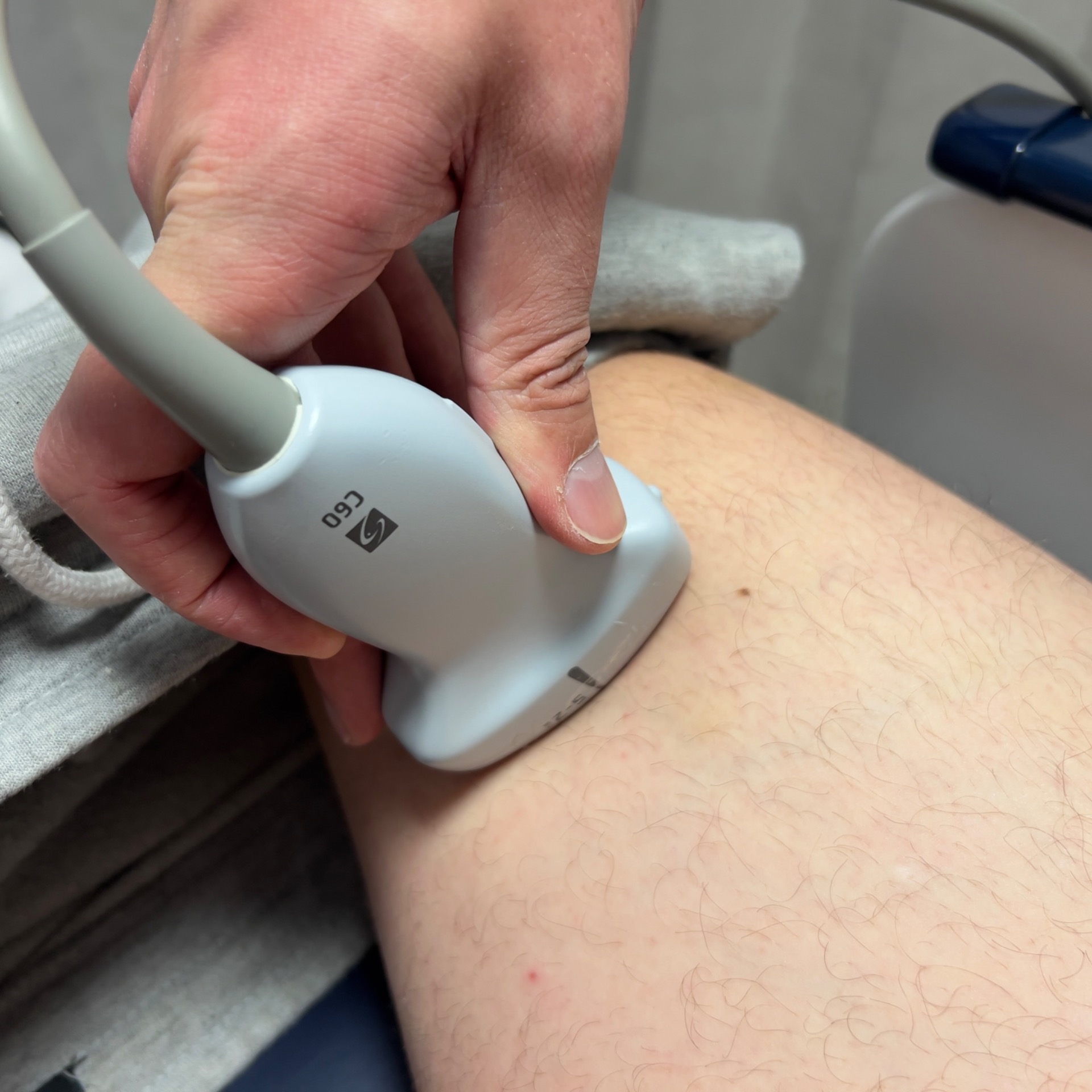
pressure against the medial femur at the adductor canal
POPLITEAL VEIN
To image the popliteal vein, flex the patient's hip and knee and image posterior to the knee in the popliteal fossa, the probe in transverse, the probe marker to the patient's right.
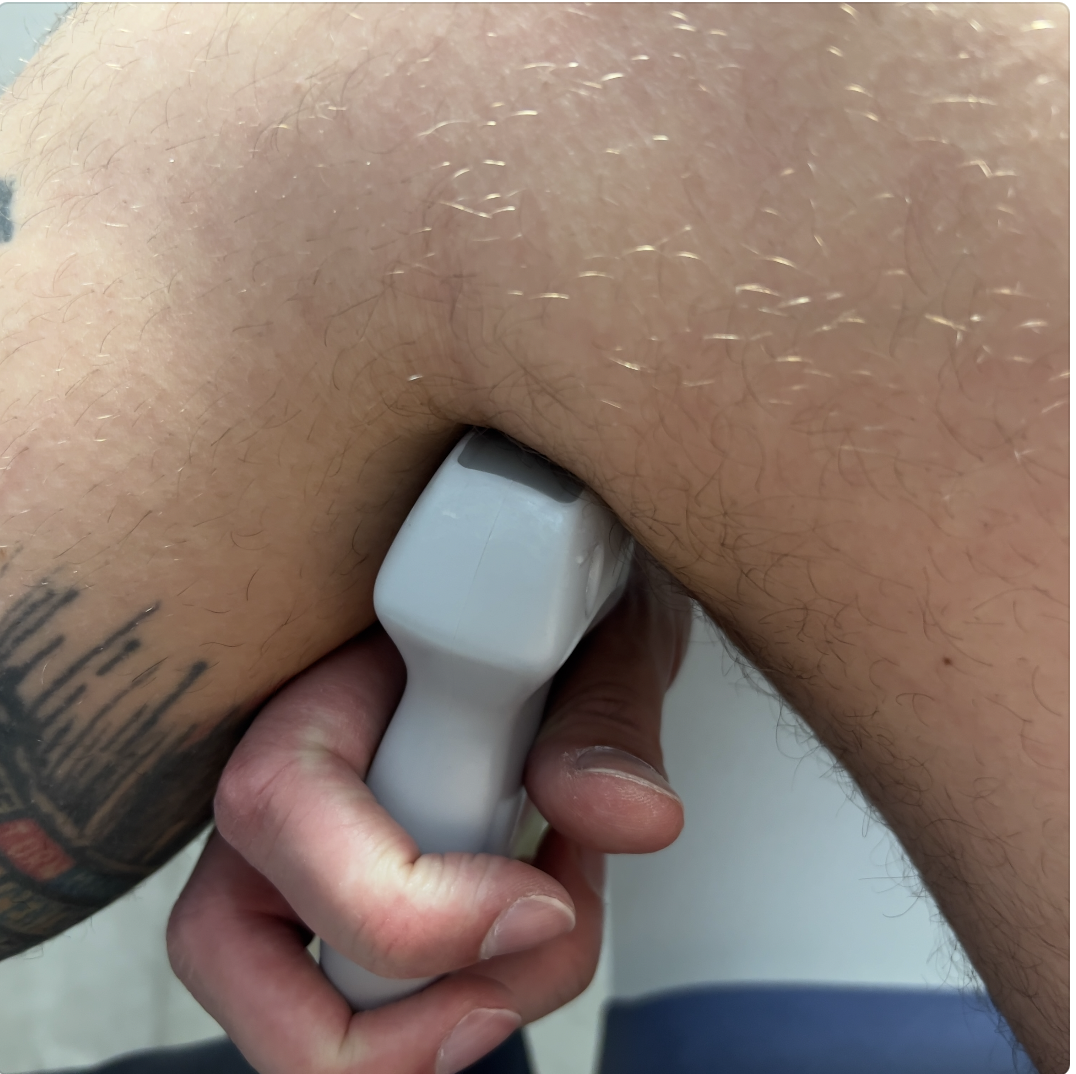
On the screen you will see the vein superficial to the popliteal artery and the tibia. Compress with upward pressure against the tibia. Fan cranially and caudally to image as much of the popliteal vein as possible.
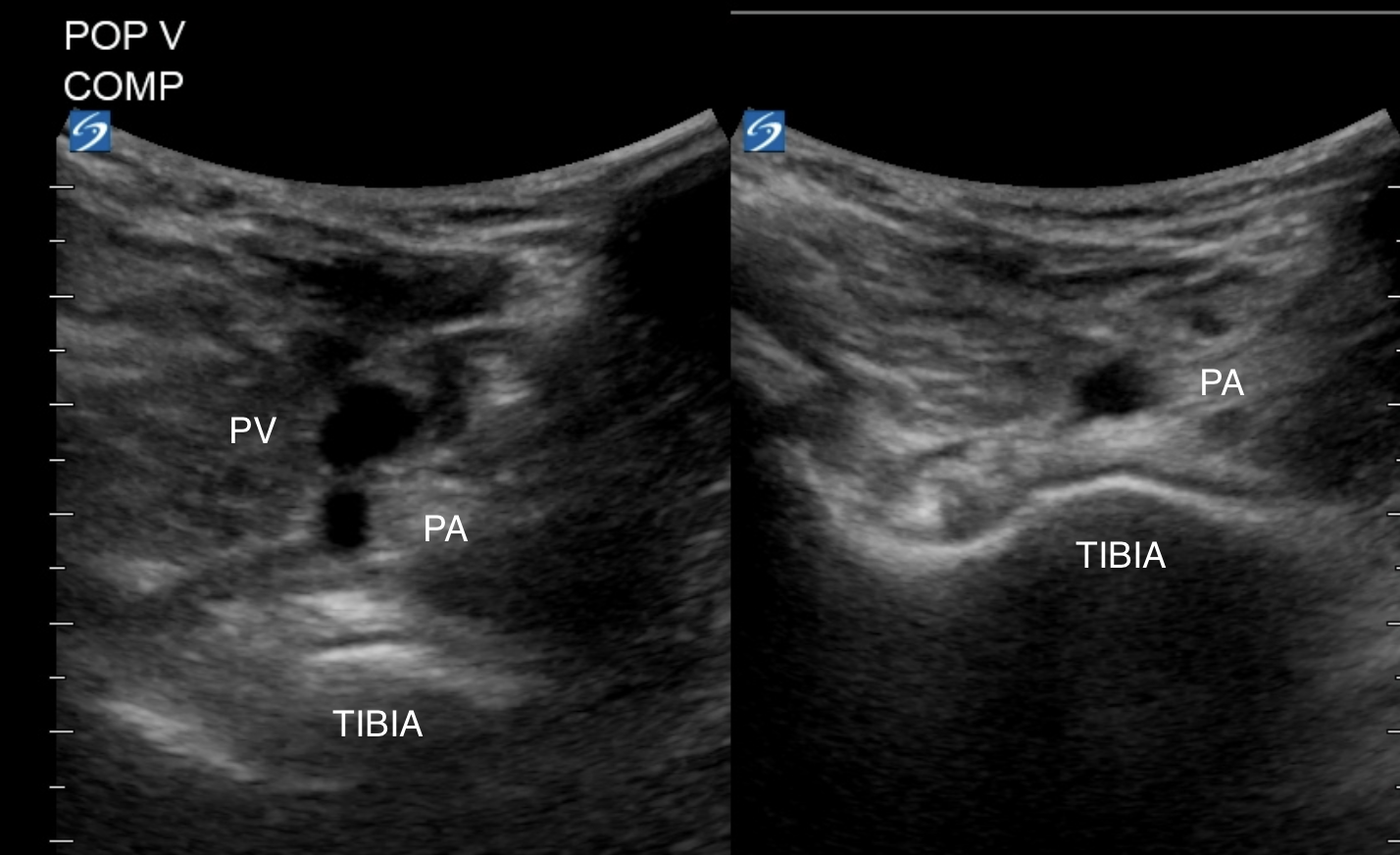
That is the end of the normal POCUS DVT exam.
Some people also look for augmentation. This is where you image a longitudinal view of the the CFV and place the PW doppler gate in its lumen. You will see venous flow as a continuous wave
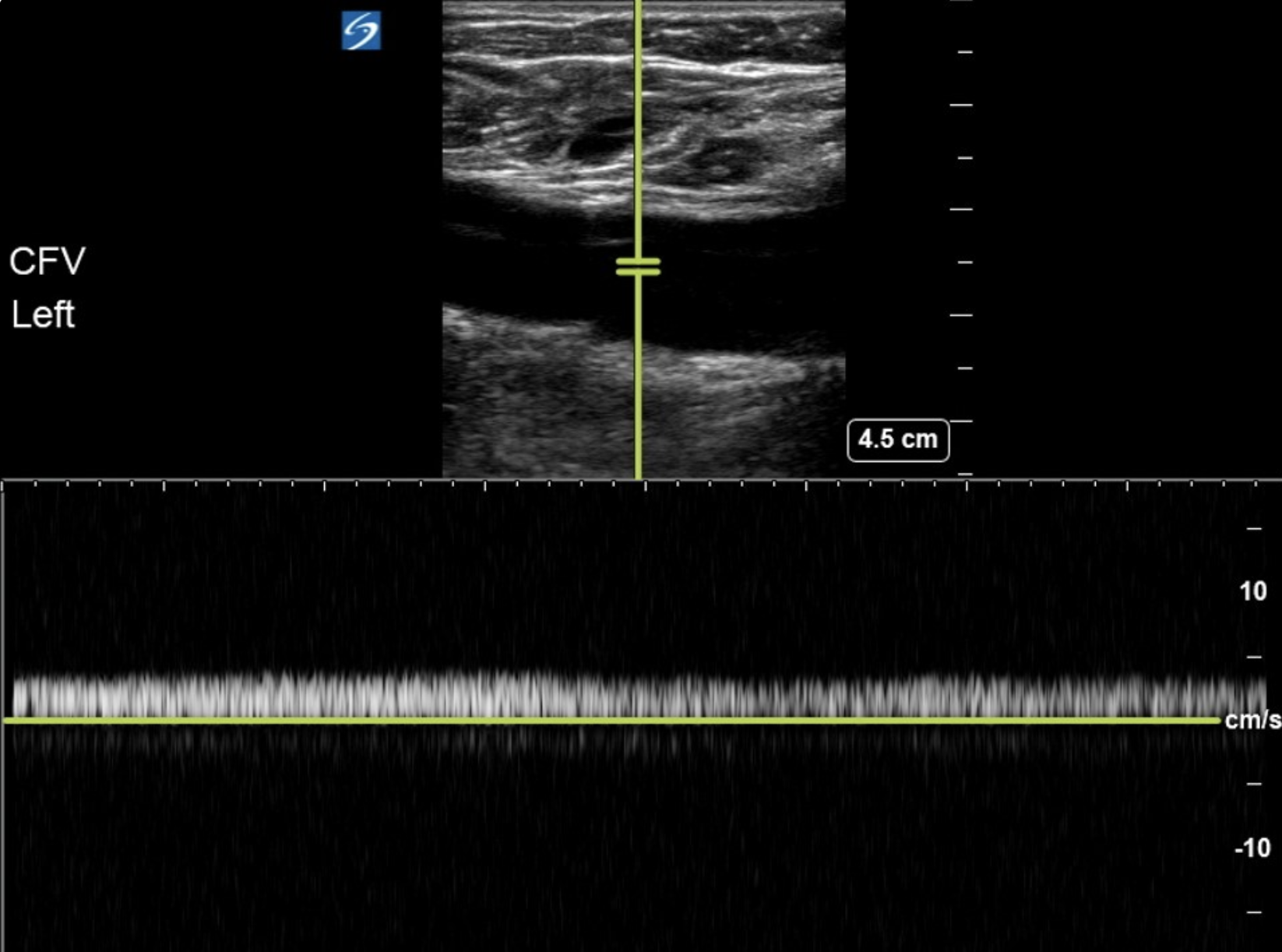
Manual compression of the calf while doing this will increase venous return and lead to enhanced flow at the time of calf compression.
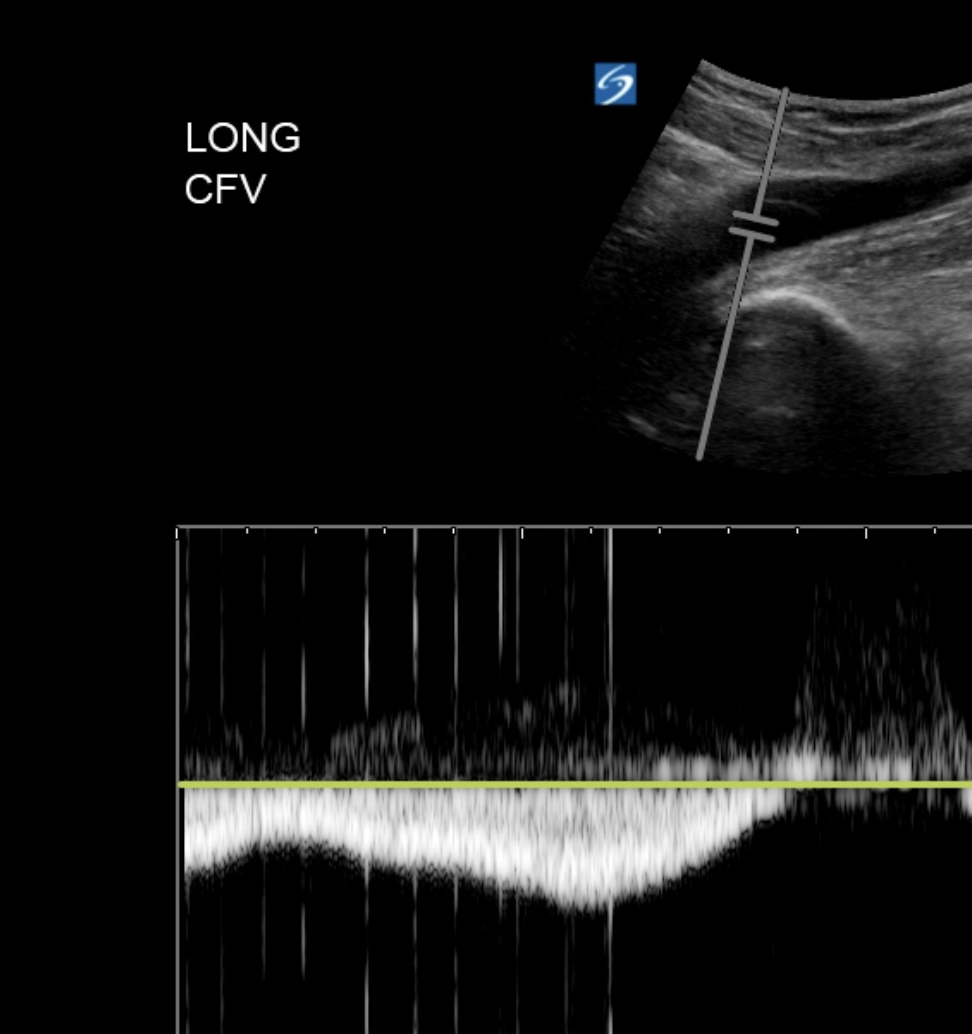
Normal augmentation of flow in the CFV due to calf compression
If the proximal veins are patent, but there is a calf DVT, augmentation won't happen or will be blunted. But the usefulness of this is questionable (4).
Another thing people do is look for respiratory variation. The CFV joins the central veins: external iliac and common iliac. Central veins show respiratory variation in flow due to the variation in right heart filling with respiration. On inspiration, venous blood is pulled into the right heart. So flow diminishes on patient inspiration in the CFV if the veins are patent up to the right atrium.
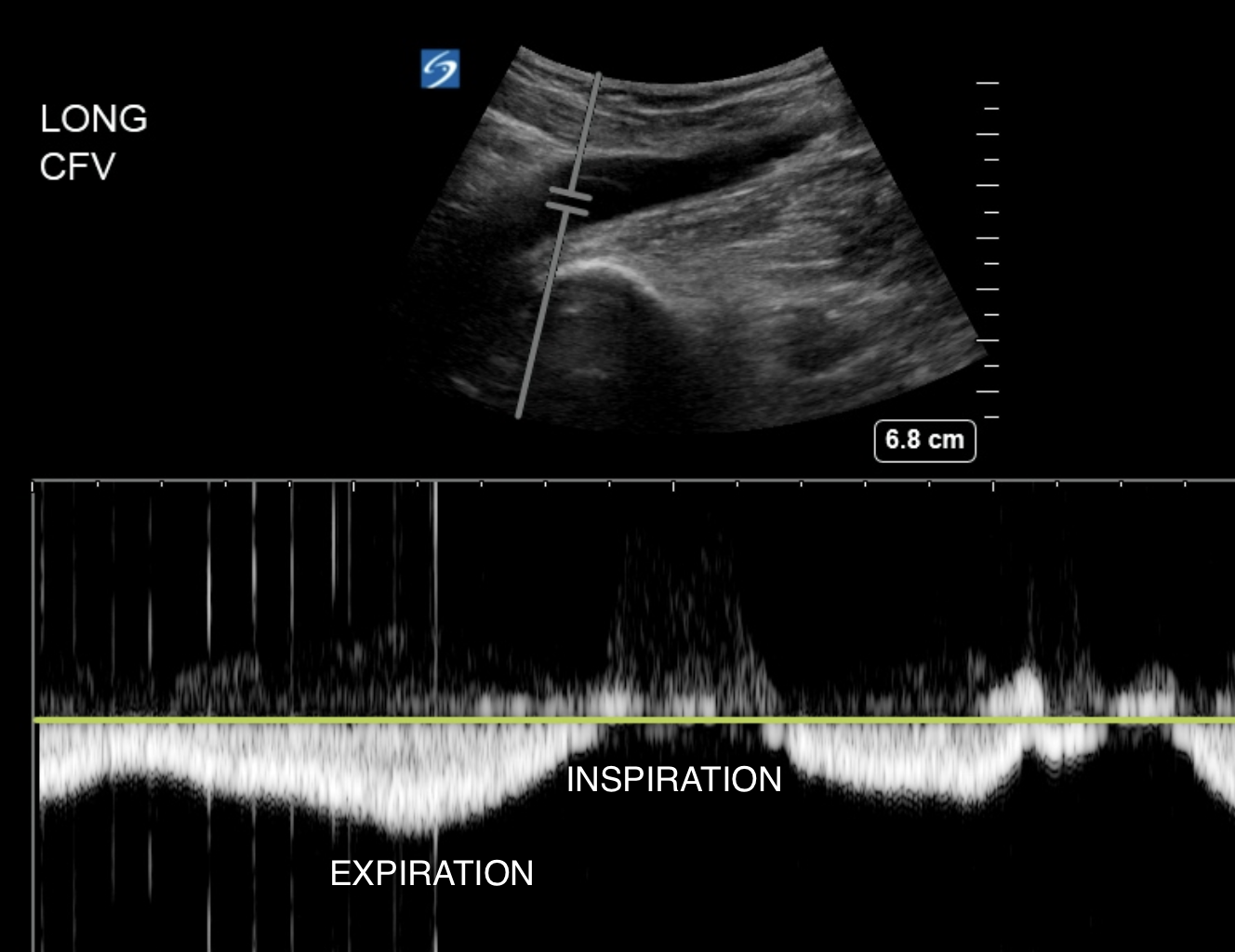
A DVT extending into the iliacs may need vascular surgery involvement and further assessment with CT angiogram for definitive management.
DVT
A vein with an acute thrombus will have echogenic material in its lumen and will be incompressible or only partially compressible.
echogenic lumen + incompressible =DVT
Clot in the CFV. The saphenous vein compresses but the CFV does not.
Sometimes you may also see echogenic fat surrounding the thrombosed vein due to inflammation.
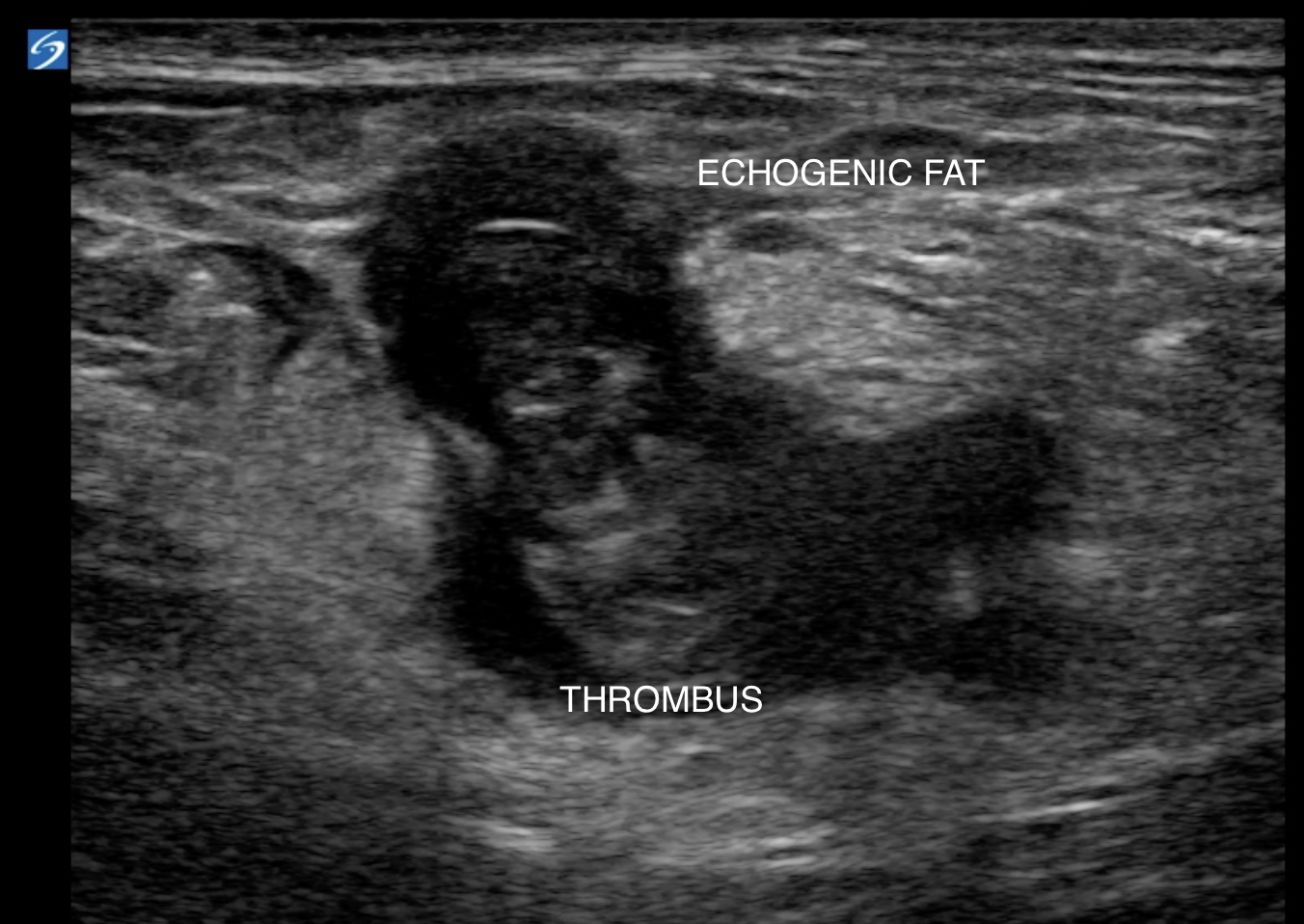
The fat surrounding the thrombosed vein appears more hyperechoic than normal
A mobile thrombus is at high risk of embolisation so try not to compress these ones too aggressively or at all!!
REFERENCES
1. Burnside PR, Brown MD, Kline JA. Systematic review of emergency physician-performed ultrasonography for lower-extremity deep vein thrombosis. Acad Emerg Med 2008;15:493–8.
2. Tabbut M, Ebersole N, Icken L, Jones R, Gramer D. Two-point Compression Ultrasound Technique Risks Missing Isolated Femoral Vein DVTs. West J Emerg Med. 2022 Jun 3;23(4):597-600.
3. Pomero F, Dentali F, Borretta V, et al. Accuracy of emergency physician performed ultrasonography in the diagnosis of deep-vein thrombosis: a systematic review and meta-analysis. Thromb Haemost 2013;109: 137–45.
4. Lockhart ME, Sheldon HI, Robbin ML. Augmentation in lower extremity sonography for the detection of deep venous thrombosis. AJR Am J Roentgenol. 2005 Feb;184(2):419-22.


